Table of Contents
This page is a summary of simple commonly asked questions.
For the FAQ encyclopedia, this is the page for you!
WHAT ARE CANNABINOIDS?
Cannabinoids are, simply put, a chemical which the body produces and for which it has receptor cells. This chemical can also be synthesized in a lab or found in the cannabis plant.
In humans, there is something called the endocannabinoid system which allows cannabinoids to bind with receptor cells throughout the body. The interaction is similar to that of chemicals like adrenaline, testosterone, estrogen, or serotonin.
The highest concentration of cannabinoid receptors is found in the brain, but such receptors are also found throughout the body in lower concentrations, notably on the cells that are responsible for immunity and inflammation responses.
HOW DOES CANNABIS WORK?
Knowledge of how the endocannabinoid system works and how it helps patients is growing. For over 50 years, there was a log-jam preventing adequate studies on the subject and researchers are only now beginning to overcome those road blocks. What has been learned is that the usage of medicinal cannabis releases cannabinoids into the human body.

These cannabinoids, which are already naturally occurring in the body, bond to receptor cells and create various beneficial reactions. In instances where they have bonded to receptors on cancer cells, they have been seen promoting cancer cell death. In cases where they have bonded to receptors within the body’s inflammatory system they have been thought to suppress inflammation reactions. The changing tides concerning the public’s general opinion on medicinal cannabis has created a push for further research, and the ongoing results continue to signal that medicinal cannabis is an ideal treatment option for many ailments.
IS MEDICAL CANNABIS SAFE?
All medical treatments carry inherent risk, but the risks associated with medicinal cannabis are lower than a majority of other options. Unlike most modern drugs – be they caffeine, aspirin, opioids, or alcohol – there is no known risk of overdose from cannabis. Studies in animals which suggested otherwise were proven to have been faked, and the US Drug Enforcement Administration goes so far as to note on their own website that no deaths from cannabis overdose have ever been reported.

Further, medicinal cannabis is safer than many other medicines because it rarely reacts to other treatments. It can be used with nearly all traditional medications without concerns for dangerous interactions. Lastly, it should be noted that medicinal cannabis is thoroughly tested and processed for microbiological contaminants, pesticides, residual solvents, and heavy metals. Physicians who recommend medicinal cannabis take safety seriously and include information concerning the testing process as part of patient education.
WHAT ARE THE DIFFERENT WAYS TO CONSUME CANNABIS?
There are three primary administration routes for medicinal cannabis: inhalation, ingestion, and application. Inhalation is the first route that occurs to most people, but many misconceptions about this option exist. When asked what they think when “inhalation” of cannabis is mentioned, most people imagine using a flame to light a dried plant in order to inhale the smoke.
This is not recommended. Combusting cannabis is not only unsafe but also less effective; the toxins released by combustion are dangerous and the temperatures from a flame are much higher than the melting point of cannabinoids. Instead, when medicinal cannabis is to be inhaled, a vaporization device is used. This limits temperatures, eliminates the need for combustion, prevents the inhalation of smoke related toxins, and uses less cannabis. Ingestion is the second most common route of administration, utilizing specific dosages in the form of prepared foods, drinks, tinctures, capsules, gum, sublingual strips, or pills. Lastly, an increasingly more common option is the application of lotions, ointments, or transdermal patches.
If your questions are specifically about children or teens, including concerns about safety, brain development, or behavior, please see Pediatric Cannabis: Honest Answers for Skeptical Parents .
IS MEDICAL CANNABIS ADDICTIVE?
Cannabis is not reported to cause physical dependence, and the withdrawal symptoms normally associated with addictive substances are minimal, if present at all. Studies suggest that, because cannabinoids are stored in fat calls, an abrupt cessation of cannabis usage results in a slow tapering effect and no withdrawal symptoms.

This is a particularly important question to ask during a time where the opioid crisis, which many believe began due to the over utilization of prescription drugs for pain management, has become a Nationwide Public Health Emergency. It is notable that medicinal cannabis is a far safer pain management option with minimal concerns over addiction and no records of death due to withdrawal or overdose.
DOES MEDICAL CANNABIS GET YOU HIGH?
Various cannabinoids affect each individual differently, and the method through which cannabis is administered can play a significant role individual effectiveness.

Generally speaking, most ingested and inhaled medicinal cannabis will have some degree of an intoxicating effect. On the other hand, most topical applications – with the exception of transdermal patches – are not able to enter the blood stream and thus do not include these effects. With experience and instruction, a person can titrate their dosage to minimize the intoxicating effects of cannabinoids. A physician with experience in the usage of medicinal cannabis can guide patients and provide a large amount of information concerning how different cannabinoids are likely to affect an individual. They can also make suggestions regarding which types of medicinal cannabis are less likely to have intoxicating effects.
Questions About Patient Rights
WHY IS MEDICINAL CANNABIS NOT LEGAL IN ALL STATES?
Cannabis was used in clinical medicine in the United States until 1937 when Congress, despite opposition by members of the American Medical Association, passed a Tax Act which effectively ended the usage of cannabis.
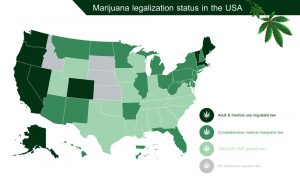
The stigma and misinformation which began in that campaign were difficult to overcome and ultimately led to a federal ban on most medical research. But now that scientists and physicians have begun studies in earnest, the medical benefits of cannabis are becoming more obvious to the public, medical practitioners, and politicians. The increasing amount of information has changed the political climate, and legislation has become more understanding of the need for further study and usage. As a result, 29 states, Washington DC, Guam, and Puerto Rico have passed bills legalizing medicinal cannabis.
CAN I BE FIRED FOR BEING A MEDICAL CANNABIS PATIENT?
Active patients of the Massachusetts Medical Use of Marijuana Program have their information protected by the U.S. Department of Health Human Services, in The Health Insurance Portability and Accountability Act of 1996 (HIPAA). Additionally, on July 17, 2017, the Massachusetts Supreme Judicial Court, in Barbuto v. Advantage Sales and Marketing, ruled that an employee fired for a positive drug test due to his/her lawful use of medical marijuana may assert a claim for disability discrimination under the Massachusetts employment discrimination statute. Also, patients and employers may refer to Section 22 of Bill S.978, An Act Relative to the Fair Treatment of Employees.
This is not to say that patients are advised to consume cannabis while at work, as this is unlawful. Nor is it lawful to ever be intoxicated during work hours. Violating such stipulations may forfeit the patient’s rights to sustained employment.
Patients who are concerned about their employment relations may reach out to CED Clinic for support though letter writing, communicating with Human Recourses and educating employers upon request. In the event of a drug-test, which can sometimes be scheduled far enough in advance that either one can choose to eliminate cannabis from the system, or with a medical card, one can discuss with employers in advance, after accepting a job or anonymously calling the HR department to inquire what their policies are.
Go To The FAQ Encyclopedia